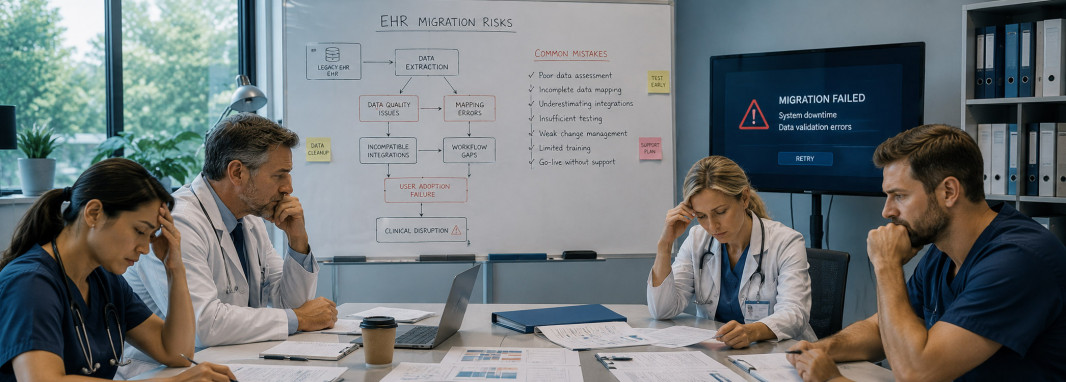
EHR migration is often treated as a technical infrastructure project.
That assumption creates expensive mistakes.
Healthcare migrations directly affect patient care, provider workflows, compliance readiness, and day-to-day operations.
A poorly managed migration can slow clinics down for weeks, damage data integrity, frustrate staff, and create long-term operational instability.
Successful modernization depends less on moving data and more on protecting clinical continuity.
Treating Migration as a Pure IT Project
One of the most common mistakes is viewing migration as something the technical team handles independently.
Clinical workflows are deeply operational.
If physicians, nurses, billing teams, and administrators are excluded from planning, the result often breaks real-world processes.
EHR modernization requires both technical architecture and operational workflow design.
Organizations planning complex modernization initiatives often benefit from a defined EHR migration strategy aligned with actual clinical operations.
Underestimating Data Cleanup Complexity
Legacy systems often contain years of inconsistent information.
Common issues include:
- duplicate patient records
- outdated demographics
- broken document references
- inconsistent field structures
- partial clinical histories
- legacy coding mismatches
Moving bad data into a new system creates a newer version of the same problem.
Migration should include cleanup, normalization, validation, and governance.
Ignoring Patient Data Architecture
Migration is not only about moving records.
It is about preserving data integrity across the healthcare ecosystem.
If architecture planning is weak, organizations often create:
- fragmented patient histories
- missing encounter records
- broken provider relationships
- incomplete reporting visibility
- data ownership confusion
Scalable secure patient data migration planning helps preserve continuity while improving long-term operational control.
Breaking Clinical Workflows During Go-Live
Some migrations focus heavily on technical delivery and neglect day-one usability.
This creates operational chaos.
Common symptoms:
- providers cannot find records quickly
- clinical notes take longer
- appointment workflows slow down
- billing handoffs fail
- staff create manual workarounds
Technical success means very little if clinical operations collapse after deployment.
Migrating Documents Poorly
Healthcare environments rely heavily on structured and unstructured documentation.
This includes:
- referrals
- lab reports
- scanned records
- signed forms
- insurance documents
- care plans
- historical attachments
Document migration is frequently underestimated.
Broken metadata, inaccessible files, missing references, and inconsistent indexing create major operational disruption.
Reliable medical document migration workflows help prevent document chaos after launch.
Skipping Real Integration Testing
Modern healthcare operations depend on connected systems.
Migration affects more than the EHR itself.
Connected systems may include:
- billing platforms
- telehealth systems
- diagnostic tools
- lab integrations
- CRM systems
- patient portals
- insurance workflows
If integration testing is superficial, failures appear in production instead of staging.
That creates avoidable downtime.
Trying to Migrate Everything at Once
Big-bang migration sounds efficient.
In healthcare, it often increases risk dramatically.
Moving every workflow, integration, document set, and historical record simultaneously creates too many failure points.
Phased migration often creates safer operational outcomes.
Weak Staff Training
Even technically successful platforms fail when staff are unprepared.
Training often gets compressed late in the project.
This creates:
- workflow confusion
- user frustration
- slow adoption
- error-prone data entry
- productivity loss
Clinical adoption is part of migration success.
No Rollback or Contingency Plan
Healthcare systems cannot tolerate uncontrolled failure.
Migration projects need contingency planning.
That includes:
- rollback procedures
- backup access plans
- temporary workflow continuity
- incident response ownership
- technical escalation paths
Without fallback planning, small issues become operational emergencies.
Ignoring Post-Migration Stabilization
Go-live is not the finish line.
Healthcare systems typically require active stabilization after launch.
This includes:
- bug resolution
- workflow adjustments
- performance tuning
- staff feedback loops
- data validation reviews
Organizations that skip stabilization often carry operational friction for months.
Final Thoughts
EHR migration failures usually come from operational blind spots rather than technical incompetence.
Healthcare modernization succeeds when architecture, workflows, data governance, integrations, compliance, and user adoption are planned together.
The safest migration strategy protects clinical operations while creating stronger infrastructure for long-term growth.